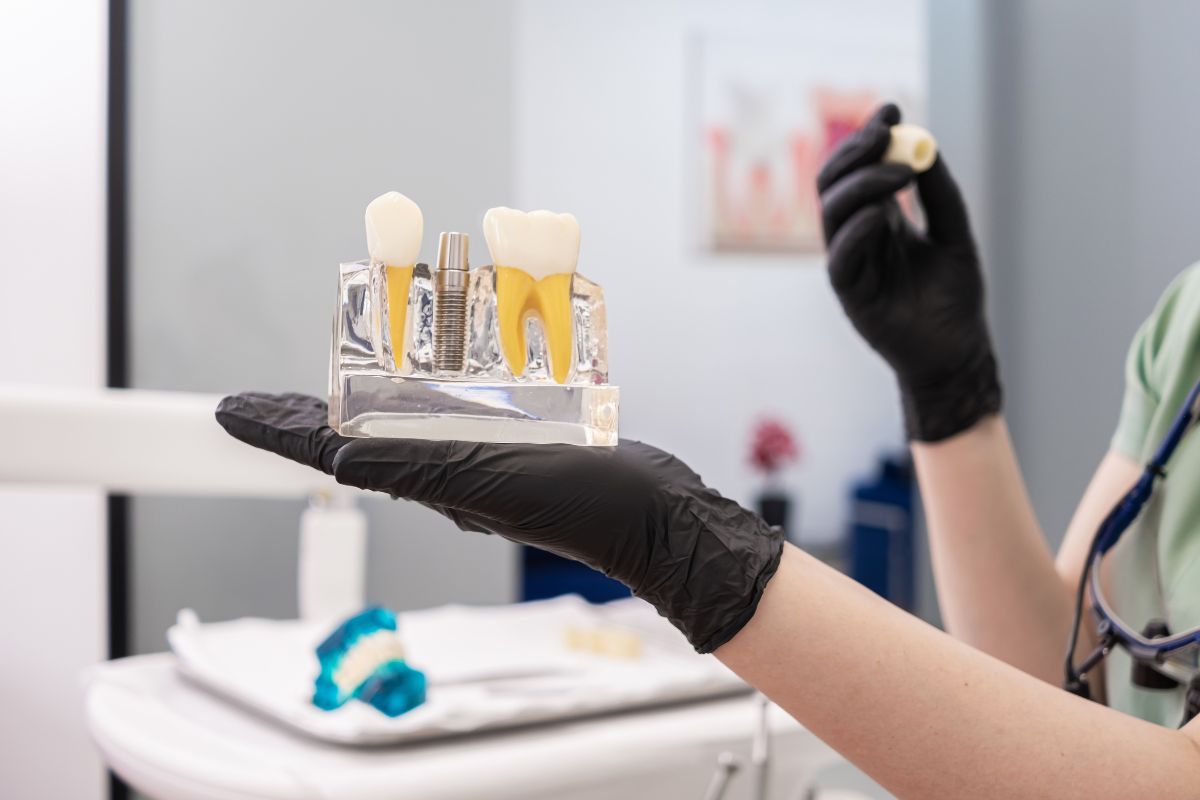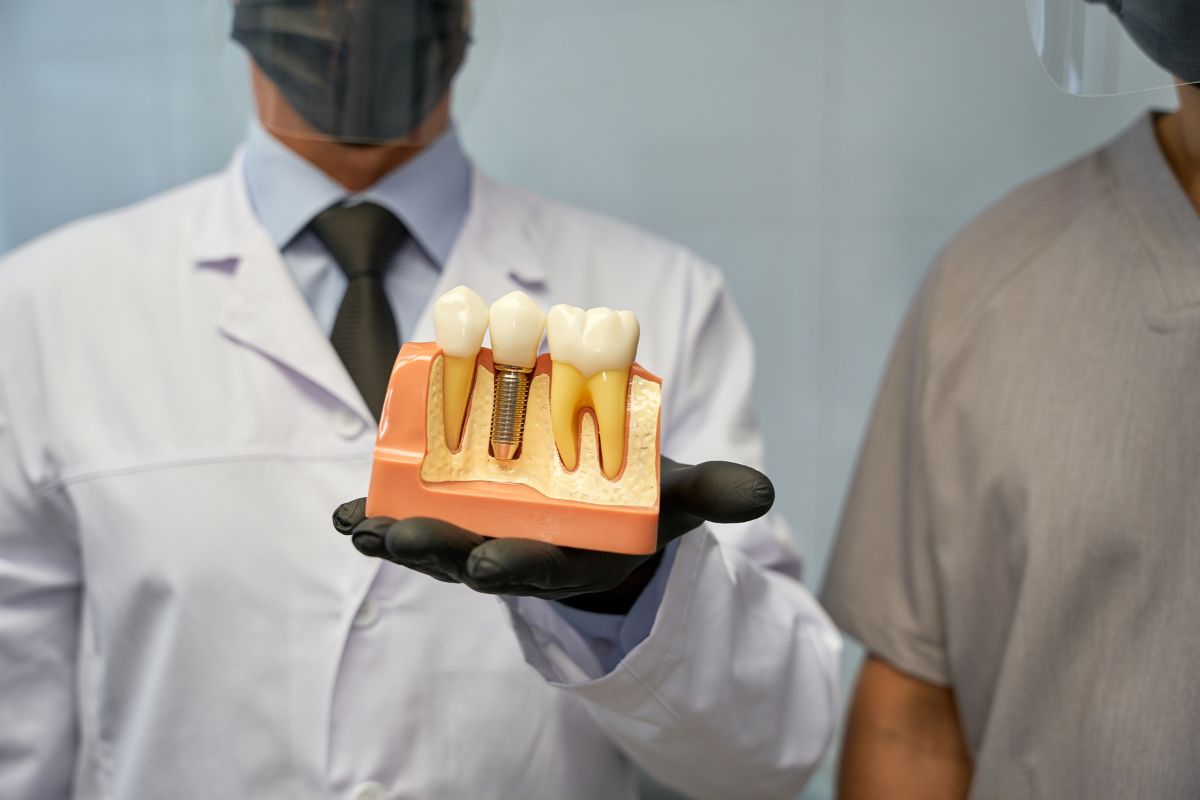
Have you ever wondered if a history of gum issues could stand in the way of restoring your smile? Many people face this question when considering options for missing teeth. Dental implants offer a natural-looking solution that feels secure and functions like real teeth. Yet, gum health plays a key role in the process. Let’s dive into what you need to know to make an informed choice.
Understanding Gum Disease
Gum disease, also known as periodontal disease, starts with plaque buildup. It leads to inflamed gums that bleed easily. If ignored, it progresses to periodontitis. This advanced stage damages the bone supporting your teeth.
Bacteria cause the infection. Symptoms include red, swollen gums and bad breath. Loose teeth often follow. Early detection matters. Regular checkups help spot it before major harm occurs.
How Gum Disease Affects Dental Implant Eligibility
Active gum disease poses risks for implants. Implants need stable bone and healthy tissue to integrate properly. Diseased gums create an unstable base. This raises the chances of failure.
Osseointegration is crucial. It’s the process where the implant fuses with the jawbone. Inflammation from gum disease disrupts this. It can lead to peri-implantitis, a condition similar to gum disease but around implants.
Not all cases are off-limits. If the disease is mild and treated, options open up. Severe cases may require extra steps. Bone loss from long-term issues often needs addressing first.
Treating Gum Disease for Implant Success
Treatment begins with deep cleaning. Scaling and root planing remove plaque below the gum line. Antibiotics may help control infection.
For advanced cases, surgery might be needed. Flap surgery exposes roots for thorough cleaning. Grafts can rebuild lost bone or tissue.
Once gums heal, implants become feasible. Healing takes time, often months. Patience pays off with better outcomes.
Maintenance is key post-treatment. Brushing twice daily and flossing prevent recurrence. Professional cleanings every few months support long-term health.
Steps to Prepare for Dental Implants
Start with a full evaluation. Your dentist assesses gum and bone health. X-rays reveal hidden issues.
If the bone is insufficient, grafting builds it up. This uses synthetic or natural material. It strengthens the area for implant placement.
Timing matters. Wait until the gums are infection-free. Rushing leads to complications.
In areas like Bel Air, MD, many seek dental implants after managing gum problems. Local expertise ensures tailored care.
Risks and Prevention Strategies
Even after treatment, risks linger. Peri-implantitis affects some patients. Signs include swelling and bone loss around the implant.
Prevention starts at home. Use soft-bristle brushes. Avoid tobacco, as it worsens gum issues.
Regular visits catch problems early. A diet rich in vitamins supports healing. Stay hydrated to reduce dry mouth risks.
Statistics on Gum Disease and Implant Outcomes
Here’s a quick look at key data to guide your expectations:
| Statistic | Detail | Source Insight |
|---|---|---|
| General Implant Success Rate | 90-98% over 10 years | American Dental Association studies show high success in healthy patients. |
| Failure Rate with Gum Disease History | Up to 10x higher than natural teeth | Retrospective studies indicate increased risks if not managed well. |
| Peri-Implantitis Prevalence | Affects 20% within 5-10 years | Common in those with prior periodontal issues without strict maintenance. |
| Survival After Treatment | 90% at 10 years | Improves significantly post-gum therapy and bone support. |
These numbers highlight why addressing gum disease first boosts chances.
Trending FAQs on Dental Implants and Gum Disease
Many search for answers on this topic. Here are some frequently asked questions based on common Google queries, with straightforward responses:
- Can gum disease be cured before getting dental implants? Yes, through treatments like scaling, root planing, or surgery. Once controlled, implants can proceed safely.
- What happens if I get gum disease after dental implants? It can lead to peri-implantitis, causing inflammation and potential implant loss. Early intervention with cleaning and antibiotics often resolves it.
- How does gum disease affect dental implant success? It weakens bone and tissue support, increasing failure risks. Treated cases see success rates near 90%.
- Are there alternatives to dental implants if I have severe gum disease? Options include bridges or dentures, but implants remain viable after gum stabilization.
- Can bone grafting help if gum disease caused bone loss? Absolutely. Grafting rebuilds bone, making implants possible even after significant damage.
These address top concerns and provide clarity.
Long-Term Care for Lasting Results
Ongoing care ensures implants thrive. Schedule biannual checkups. Monitor for any gum changes.
Lifestyle choices matter. Quit smoking to improve healing. Balanced nutrition aids tissue repair.
If you notice issues, act fast. Early fixes prevent bigger problems.
If you are searching for a reliable implant dentist in Bel Air, MD, consider one with experience in handling gum-related cases for personalized guidance.
Restoring your smile after gum challenges feels empowering. With proper steps, dental implants can transform daily life. They boost confidence and comfort. Embrace the journey toward better oral health today.